Let us help you breathe easier.
Respiratory care specializes in treating individuals suffering from breathing and cardiac disorders. Windom Area Health staffs a Respiratory Therapist who is trained on advanced respiratory medical equipment and who works closely with patients to help them manage their conditions.
For more information, give us a call at 507-831-0647.

Pulmonary Rehabilitation
Pulmonary rehabilitation is a program that combines education and exercise to help you manage your breathing problem, increase your energy level and decrease your feeling of breathlessness. During the education portion of the program you will learn about your lung disease and how to become more “in charge” of your breathing instead of your breathing being “in charge” of you. You’ll become stronger by increasing your level of fitness. Exercising your lungs and muscles will help you be more active so you can continue to do the things you enjoy. Pulmonary rehabilitation may even decrease the need for hospital visits.
Your Pulmonary Rehab team will include, but not be limited to, a medical doctor, a respiratory therapist, a pharmacist, dietitian, and social worker. Together these healthcare professionals create a personal program to meet your specific needs.
Pulmonary rehabilitation is recommended for patients with lung disease who experience shortness of breath frequently and are not able to perform daily activities despite daily use of medication. Many patients in rehabilitation programs have a diagnosis of COPD, but these programs also help people with other types of chronic lung disease that limits breathing and activity.
- Education about your disease
- Learn about your medication
- Reduce the feeling of air hunger with activity
- Healthy eating habits
- Build up some strength and learn to stay active
- Psychosocial support
Some of the education topics could include:
- Breathing retraining
- Lung disease
- Staying Healthy
- Review of medication
- Nutrition
- Dealing with anxiety, stress, depression and coping with lung disease
- Activities of daily living
- Energy conservation
- Advanced directives
The cost to you depends on your insurance coverage. Medicare covers pulmonary rehabilitation for COPD, if you meet certain requirements. Medicare may also cover rehabilitation for other lung diseases, but that depends on your coverage. The pulmonary rehabilitation program coordinator, along with the hospital billing department, can assist you in reviewing your coverage and let you know what your costs will be.
Typically classes meet 2-3 days per week for an average of 4-12 weeks. The classes are offered either in a group setting so you get the chance to meet others with your condition or may be individually structured to meet your needs.
You will need to be referred by a medical doctor for the program. A thorough assessment of your medical history will determine your qualification for the program. Once accepted, a patient-tailored plan will be developed which will include, but not be limited to, exercise training, individualized education topics and behavior changes to help you manage your lung disease better.
Pulmonary Function Tests
Pulmonary Function Tests (PFTs) are noninvasive tests that show how well the lungs are working. The tests measure lung volume, capacity, rates of flow and gas exchange. Your healthcare provider can use this information to diagnose and treat certain lung disorders.
There are two types of disorders that cause problems with air moving in and out of the lungs:
- Obstructive: air has trouble flowing out of the lungs due to airway resistance. This causes a decreased flow of air.
- Restrictive: the lung tissue and/or chest muscles cannot expand enough. This creates problems with airflow, mostly due to lower lung volumes.
Pulmonary Function Tests can be done with two methods. These methods may be used together and perform different tests, depending on the information that your healthcare provider is looking for:
- Spirometry: a simple test to measure how much (volume) and how fast (flow) you can move air in and out of your lungs.
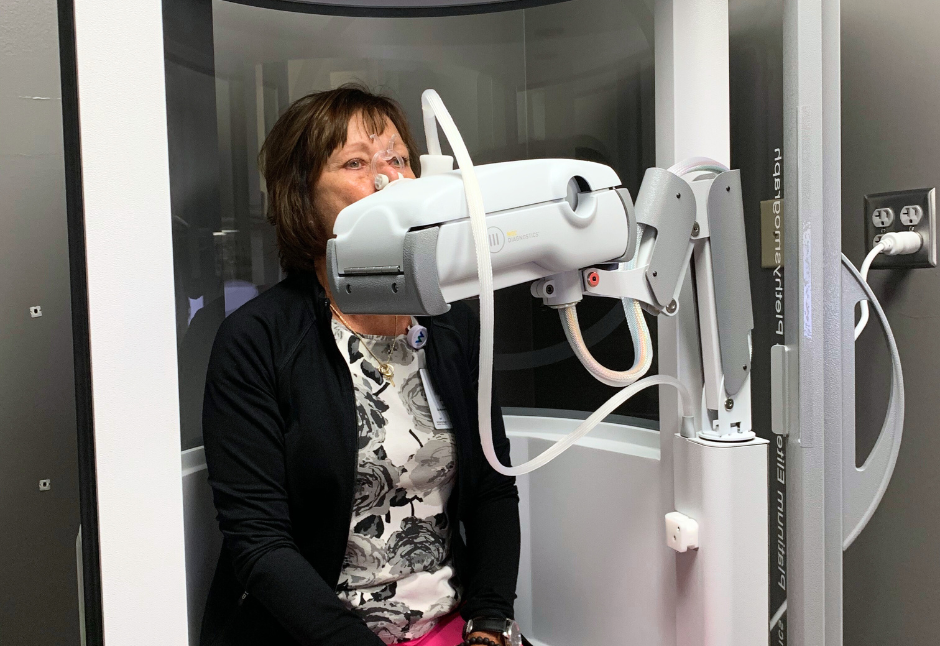
- Plethysmography: this test is used to measure how much air you can hold in your lungs. You will sit inside an air-tight box that looks like a short, square telephone booth to do the tests.
There are many different reasons why Pulmonary Function Tests (PFTs) may be done.
- They are sometimes done in healthy people as part of a routine physical
- They are routinely done in certain types of work environments to ensure employee health (such as graphite factories and coal mines)
- PFTs may be used to check lung function before surgery or other procedures in patients who have lung or heart problems, who are smokers, or who have other health conditions
- To assess treatment for Asthma, Emphysema and other chronic lung problems
A healthcare provider may order Pulmonary Function Tests to help diagnose health problems such as:
- Chronic lung conditions such as asthma, bronchiectasis, emphysema or chronic bronchitis
- Restrictive airway problems from scoliosis, tumors, or inflammation or scarring of the lungs
- Trouble breathing from injury to the chest or a recent surgery
- Asbestosis, a lung disease caused by inhaling asbestos fibers
- Respiratory infections or allergies
Because Pulmonary Function Testing is a noninvasive procedure, it is safe and quick for most people. The person must be able to follow clear, simple directions.
All procedures have some risks. The risks of this procedure may include:
- Dizziness during the test
- Feeling short of breath
- Coughing
- Asthma attack brought on by deep inhalation
In some cases, a person should not have PFTs. Reasons for this include:
- Recent eye surgery, because of increased pressure inside the eyes during the procedure
- Recent belly or chest surgery
- Chest pain, recent heart attack or an unstable heart condition
- A bulging blood vessel (aneurysm) in the chest, belly or brain
- Active Tuberculosis (TB) or respiratory infection such as a cold or the flu
Your risks may vary depending on your general health. Ask your healthcare provider which risks apply most to you. Talk with him/her about any concerns you may have.
At Windom Area Health, we utilize the MedGraphics Diagnostics Platinum Elite System for testing. We achieve accurate and validated test results that meet ATS (American Thoracic Society) and ERS (European Respiratory Society) standards.

